As I posed for pictures at the official launch of my debut book, holding a bouquet of flowers and wearing a new red evening gown, I felt on top the world.
It was September 2019, and that night was the culmination of years of painstaking reporting, research and writing. As the wine and conversation flowed, and I stood surrounded by smiling friends, peers and family, the future seemed bright.
Just seven weeks later, that night – and sense of contentment and endless possibility – had shrunk to a distant memory, as I found myself sitting in the stark, clinical office of a gastroenterologist, being told it was highly likely that I had bowel cancer.
“I couldn’t even get past it with the probe,” the female specialist said, referring to a large tumour she’d just discovered in my colon.
“Is it… cancer?” I ventured.
“I can’t know for sure until the biopsy results…but it does seem to show signs of malignancy,” she replied gently, holding up an ominous picture she had taken with a tiny camera of the white, twisted tumour, buried deep within a part of my body I’d never previously given much thought.
In that moment I didn’t understand why her mouth was still moving. I didn’t understand how I could still hear the footsteps of the nurses and doctors walking past the door. Why was the earth still turning on its axis, when my world had just ground to a halt?
In that moment I didn’t understand why her mouth was still moving
How could I possibly have bowel cancer? Surely, I was too young? As a 44-year-old working mother, I felt as though I was in the prime of my life. Although I’d suffered from sporadic pain in the left side of my abdomen for months, my GP had dismissed it as a likely infection and sent me off with antibiotics.
While it’s true that bowel cancer is widely known for affecting people aged over 50, I soon came to discover that 10 per cent of bowel cancer sufferers are actually under 50 – and that numbers are rising among younger Australians. In the past two decades, bowel cancer rates have almost doubled in 20-somethings, and have jumped by a third in those aged 30-39.
Today, it’s thought to be the deadliest cancer for men aged 30-34 and women aged 24-34, with the devastating consequences of the disease illustrated by the death of the US actor Chadwick Boseman, who lost his life to bowel cancer earlier this year at just 43 after a secret four-year battle.


Part of the problem is that bowel cancer is often detected far too late. According to Bowel Cancer Australia, which runs the Never2Young initiative, providing awareness and resources for younger sufferers, most bowel cancers start as benign, non-threatening growths – called polyps – on the wall or lining of the bowel.
If they’re caught early, polyps are usually harmless and easily removed; however, some types can become cancerous if left undetected. Too often, the cancer is only discovered once it has spread to other parts of the body, and progressed too far to treat.
My own cancer was confirmed just days after the discovery of my colon tumour.
But the bowel surgeon overseeing my case, at Cabrini Hospital in Malvern, had more bad news share: I had several metastatic tumours on my liver, he explained.
I put my hands in my head and fell forward, leaning on his desk, while my husband stared ahead in shock, turning so white his skin was like alabaster against his black polo top.
And so began a 10-month descent into the harsh, perilous and frightening world of aggressive cancer treatment.
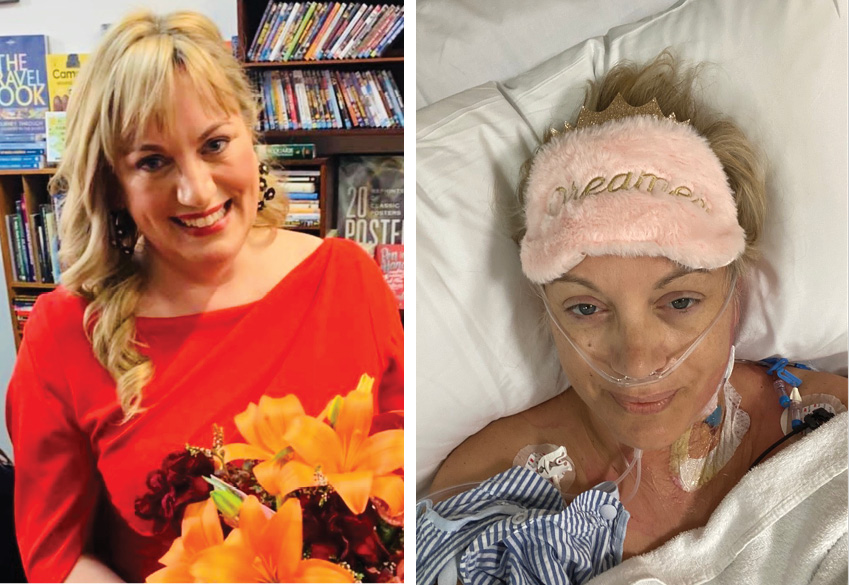

As 2019 drew to a close, I embarked on a gruelling regime of chemotherapy and surgery, complicated by infections. Then, as COVID-19 gripped the country, I spent weeks in Cabrini without seeing my children Nathaniel, 12, and Talia, 10, due to health restrictions.
In the end I’d lose so many body parts in surgery it felt like a reverse jigsaw puzzle. Half my liver was removed, along with my gallbladder, and two weeks after the operation I suffered a bowel perforation near the primary tumour. An infection developed which could have claimed my life within days due to septic shock. As a result I had a 25cm section of my sigmoid colon removed, a hysterectomy and a bladder resection.
And there were some close calls; at least twice I had to trust my instinct to go back to hospital because I knew something wasn’t right. It was so tempting to lay down and sleep, but each time the decision to get up and get help saved my life. (Always tell anyone you know with cancer they are strong, it really does help mentally in the moments when you feel weak.)
Twice I had to trust my instinct to go back to the hospital because I knew something wasn’t right
“I wish it was me suffering, not you,” my son said with tears welling in his eyes as I struggled to finish my final round of chemotherapy during Melbourne’s strict Stage Four lockdown. We were at home and completely cut off from our friends, our support network and the world around us. We turned to mindful pursuits to get through the difficult days together; we transformed the grassy council strip outside our house into an enchanted garden, we made scented candles and baked. As I grew stronger, we would take walks in the park and on the beach.
Thankfully, the results of a CT scan that I received this week revealed that all the treatment I received was worth it – that I’ve completely beaten stage four cancer. When I received the diagnosis, it felt as though I could breathe for the first time in a year. I’ve never been so appreciative of my health as I return to cycling, kayaking and enjoying life to the full. Naturally, I will have to undergo regular check-ups for years to come, but for now it feels like a very welcome miracle.
However, the experience has left me determined to raise awareness and to investigate the rise of bowel cancer in younger Australians – and the problem of misdiagnosis by GPs.
“It is alarming,” says Associate Professor Graham Newstead, head of the Colorectal Unit at the Prince of Wales Private Hospital in Sydney of the surge in early onset bowel cancer.
“My youngest patient was in her early thirties, with no family history or genetic syndrome. We also see a number of women who are pregnant and [presenting] with some bleeding, which has incorrectly been attributed to hemorrhoids rather than being investigated to exclude bowel cancer.”
It is alarming. My youngest patient was in her early thirties, with no family history or genetic syndrome.
As I became part of the wider online bowel cancer community and made friends with other sufferers, I would hear many similar stories of terrifying misdiagnosis.
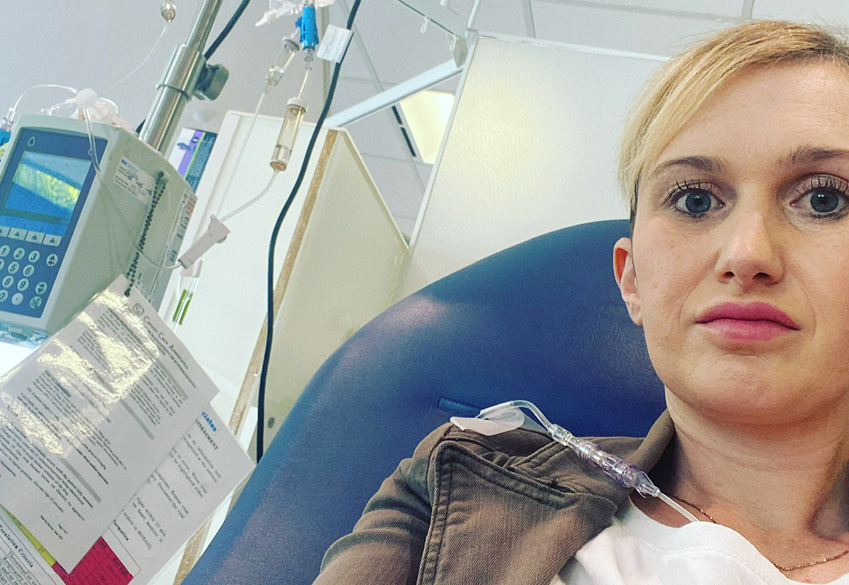
Like me, Gemma Farquhar, 35, was a busy working mother who never imagined she would face a tough fight against bowel cancer.
The human resources manager, who has two daughters, Phoebe, six, and Lily, four, had felt unwell, on and off, for two months but doctors, as well as a specialist, suggested her symptoms were likely due to food intolerances, or irritable bowel syndrome (IBS). Eventually the specialist sent her for a CT scan.


When the health-conscious Farquhar, who exercises at the gym several times a week, received a phone call saying the scan had revealed a large cancerous tumour blocking her colon she was “shocked to the core.”
“I got the call and almost collapsed,” Farquhar explains. “I had never even considered bowel cancer as a possibility for someone as healthy and young as I was, I honestly just viewed it as an old person’s disease.”
After emergency surgery, she embarked on a cycle of chemotherapy before another tumour was discovered on one of her ovaries. After a second surgery, she is now completing an additional six rounds of chemotherapy.

As I heard more shocking stories of bravery and suffering, an obvious question arose: if cases are rising among younger age groups, why isn’t the government extending the National Bowel Cancer Screening Program (NBCSP) to those under 50?
As it currently stands, every Australian is posted a bowel-testing kit (or Faecal Immunochemical Test or FIT) in the mail as soon as they turn 50, and then every two years onwards. If they score a positive result, they are sent for a colonoscopy, a procedure to see the lining of the whole large bowel using a flexible tube containing a camera and a light.
For the past two years the American Cancer Society has been calling for screening to start at 45 given the rising rates in younger people. More recently, the US Preventive Services Task Force began campaigning, too. In New Zealand, calls are growing for the government to offer earlier testing for Maori, who are more likely to suffer from bowel cancer at an earlier age.
Julien Wiggins, CEO of Bowel Cancer Australia, believes that testing should be lowered in Australia, with free kits sent to anyone over the age of 45. “We need to start screening people from age 45, while also increasing participation rates among those aged 50 and over,” he told PRIMER.
We need to start screening people from age 45
Recently, the charity commissioned a special report by social demographer Bernard Salt in which he argued that earlier screening would provide protection to an additional two million Australians, and reduce bowel cancer deaths.
Importantly, Wiggins says, there also needs to be more widespread awareness of the symptoms of bowel cancer among young people, including rectal bleeding, bloating and pain. He adds that researchers are still investigating why rates are rising among young people but that poor diets and sedentary lifestyles are suspected to be part of the equation.
Many experts are concerned that COVID-19 could see a spike in bowel cancer – with people due to have routine colonoscopies or experiencing symptoms delaying appointments or hospital visits because of fears of the virus.
I personally would like to see the government screening kits sent out from at least the age of 40. In the meantime, Prof Newstead says those aged 40 and upwards should seriously consider purchasing a screening test from their local pharmacy and encourages everyone to make bowel cancer a “dinner table” conversation.
Women, he says, need to be aware of the signs and symptoms as much as they are for other cancers, such as breast and skin cancer. “Bowel cancer is the only major cancer that has a pre-malignant condition [polyps] that we can find and remove to prevent the cancer and, even with early cancer, treat and cure.”
As I prepare for Christmas with my children, putting up decorations and planning social events with close friends, I appreciate every tiny joyous moment, remembering how I feared that last year’s celebrations, in the dark days following my diagnosis, could be my last.
Knowing how close I came to losing everything is now my motivation to help raise awareness, using my experience as a journalist and a survivor to advocate and ask tough questions where necessary.
For if I’m able to help even just one person avoid my hellish, near-fatal collision with bowel cancer it will be the best Christmas gift I could ever receive.
Want more stories like this? Sign up to our (free) weekly newsletter here.
Do you know the signs of bowel cancer?
A change in bowel habits
Blood in stools or rectal bleeding
Gas, abdominal pain or cramps
Bloating
Tiredness, weakness or weight loss
For more information about bowel cancer and its symptoms, please visit Bowel Cancer Australia













1 Comment