One weekend in November, 2015, Naomi Williams made the two-hour trip from her home in the small town of Tumut to Canberra, where her mum, Sharon, lived. At the time, Naomi was 16 weeks pregnant with her first baby, a boy, and the nausea she’d felt throughout her pregnancy was yet to abate.
But during the two days they spent together, Sharon, a Wiradjuri woman, couldn’t shake the feeling a feeling of foreboding that seemed unrelated to Naomi’s general air of malaise. “I had this awful feeling that something was going to happen to her,” she says.
In fact, throughout 2015, Naomi, a well-regarded social worker, had suffered with severe vomiting and nausea, which had begun even before her pregnancy, and her physical distress was compounded by frustration that doctors weren’t taking her health issues seriously.
Those concerns were well-founded. Hospital records would later confirm that Naomi visited Tumut Hospital and nearby doctors 20 times during 2015. Yet she was never referred to a specialist or obstetrician.
Instead, at midnight on New Year’s Eve that year, as the rest of the nation partied, Naomi – pregnant and in pain – drove herself to the Tumut Hospital emergency department. That night, she was only seen for about half an hour and sent home with two Panadol.
The next day, Naomi died of Septicaemia associated with the bacterium Neisseria meningitides – a preventable death that could have been treated with antibiotics. Her unborn baby died with her.
A coroner’s court report later ruled that although there no direct link could be made between Naomi’s ongoing vomiting and her death, there were clear and ongoing inadequacies in her care at Tumut Hospital. The Coroner found that this likely led to Naomi having “reduced expectations of care” on the night before her death, and urged the hospital to review the way it cared for Indigenous patients.


When African American man George Floyd died under the knee of a police officer earlier this year, the world coalesced in outrage over the senseless deaths of black men and women at the hands of the justice system.
In Australia, Aboriginal people were quick to point out that this callous indifference to the brutalisation of black bodies was not just an American phenomenon; the devaluation of black lives was a reality here, too, and had been for some time.
But as the waves of outrage filled the roads of capital cities, Sharon Williams sat and wondered “What about my daughter, too?”
In Australia, more than a dozen studies have revealed that far from being confined to the justice system, institutional racism is common within the health sector, too.
Indigenous Australians are one third less likely to receive the same care as other Australians. They wait longer to receive elective surgery, and have poorer survival rates from cancer, because they’re less likely to be referred to a specialist and wait longer for surgery. One in three Aboriginal or Torres Strait Islanders report that they experience racial discrimination in the health system “most” or “all” of the time.
It’s a situation that’s not unique to Australia; research has uncovered racism in the health systems of New Zealand and the US, too. However, it’s an issue that rarely receives widespread attention, and, even then, only in the most tragic of circumstances.
Two years after Naomi Williams’ death, six-year-old Charlie Gowa, a Torres Strait Islander boy, died of “overwhelming sepsis” in 2017 after being turned away from a remote Queensland hospital six times. In August 2020, the Queensland Health Ombudsman found that Charlie’s care was “not culturally sensitive” and that doctors had not adequately recognised his mother’s growing alarm.


Sharon Williams is all too familiar with the anguish of watching a child suffer.
When she died, Naomi was known for being an outgoing, caring and community-minded woman with a keen passion for social justice, a trait she inherited from her mother. An award-winning disability worker, Naomi had always been concerned about society’s most vulnerable.
But even though Naomi worked in the health sector, and her grandmother had worked at Tumut Hospital, when she fell ill, she struggled to make her concerns heard. “She would say ‘they’re not listening to me,’ ‘They don’t believe me’” recalls Sharon. “She said ‘They think I’m a drug addict.’ They were judging her, telling her ‘it’s all in your head, you’ve got drug and alcohol issues… She felt they thought she was lying to get pills. (It was later found that she was not a drug addict; she used marijuana occasionally to deal with her pain.)
In July 2015, concerned about her daughter’s welfare, Sharon wrote to the acting multi-service manager at Tumut, stating that Naomi’s illness was being overlooked.
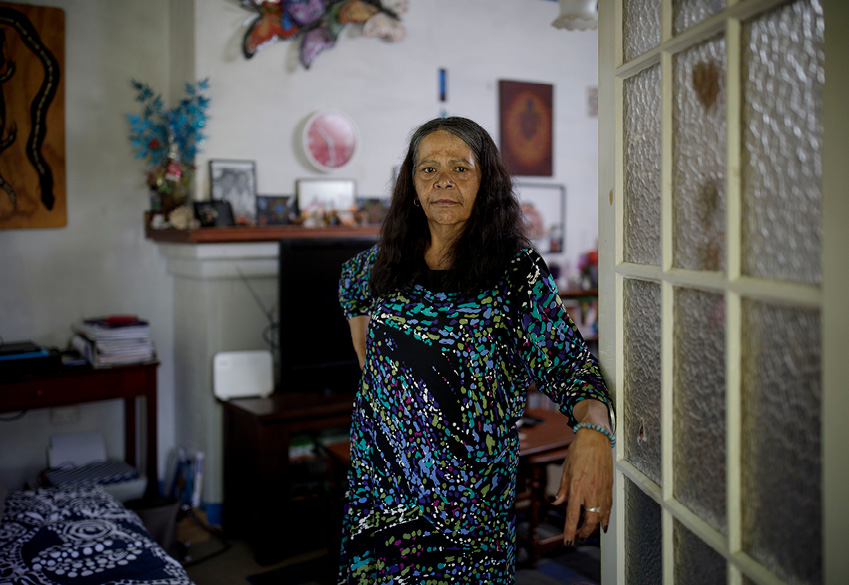
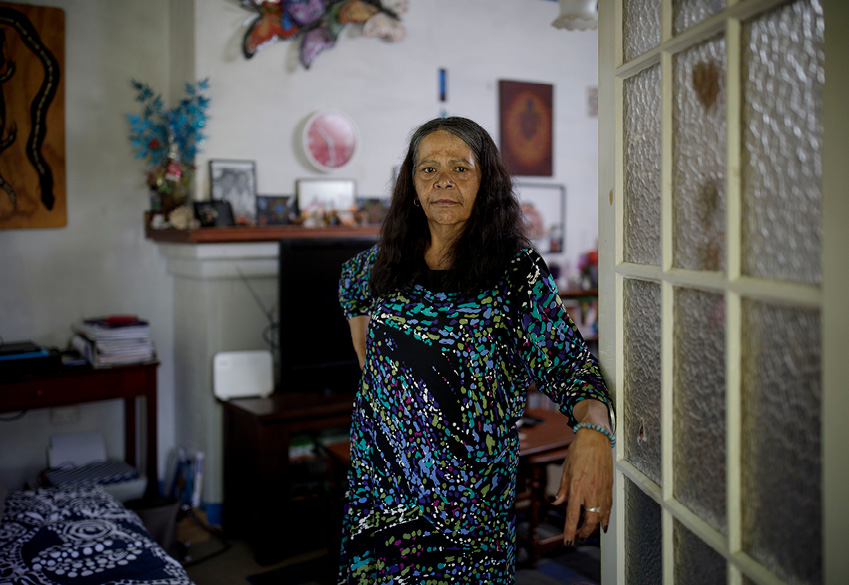
She complained that the hospital was stereotyping Naomi “as some sort of drug addict” and that the continual referrals to drug and alcohol services were “adding extra stress on her’. She also specifically asked for a specialist referral for Naomi’s condition. But that never eventuated.
Instead on New Year’s Eve 2015, Naomi arrived at Tumut Hospital, where nurses examined her for just 35 minutes before discharging her. Naomi then drove home, where her symptoms grew worse – until she suffered a seizure and an ambulance was called. By then it was too late.
Deputy state coroner Harriet Grahame found that Naomi’s previous treatment at Tumut hospital had impacted her willingness to present for care earlier in the day she died, and that there was a bias in the way she was treated by hospital staff.
She noted that it was necessary to consider Naomi’s care within the “well-known disparity between the health outcomes” between Aboriginal and non-Aboriginal people, and made nine recommendations to Tumut Hospital, including seven that were aimed at reducing “implicit bias” within the hospital.
Indigenous health researcher and Associate Professor at the University of Queensland Chelsea Bond says the issue of racism within the health system has been overlooked for too long.
“I just really feel for Naomi’s mum and having to bury a daughter and her grandchild that she never got to meet, when she should have. This was preventable. And I don’t know how we can not be more outraged, and not just outraged, but outraged into action, to do something better.’
I just really feel for Naomi’s mum and having to bury a daughter and her grandchild that she never got to meet
Dr Bond says that although the Black Lives Matter movement has raised awareness of racism within the justice system, so far, the health system has escaped similar scrutiny. “We should be equally outraged as the deaths in the hospital, in the ambulance, as we are in the watch house and the prison.”
“Colonial violence includes not treating someone properly, not investigating their conditions, not giving them the right medication, turning people away from emergency departments. That’s violence. And it’s as violent as holding people down.”
Dr Bond has been outspoken in her criticism of the government’s Closing The Gaps initiative, and in August led a group of medical experts in calling for a stronger health justice framework.
The group would like to see a foregrounding of Indigenous sovereignty in health policy “not as partners, but as architects”; funding for research into racism in health; and an awareness-raising campaign to help Aboriginal and Torres Strait Islander people seek legal support over racial discrimination within the health system.
In a paper in the Medical Journal of Australia, Dr Bond described these strategies as “small steps” towards “shifting the blame of failure for good health from Black bodies and instead demanding structural and individual health reform”.
The proposal was welcomed by many in the health sector, but comes too late for the families of Naomi Williams and Charlie Gowa.
Charlie was just six years old when he died after suffering ‘overwhelming sepsis’ stemming from melioidosis, a rare infection found in tropical climates and which disproportionately impacts Aboriginal and Torres Strait Islander people.


I tried so hard to get my son the help that he needed. The hospital would not help him and there was nowhere else we could go.
His parents first became concerned about Charlie in early January 2017 when he fell ill with body aches and diarrhoea that didn’t look normal. They took him to Bamaga Hospital, in the northern tip of Queensland, where he was sent away with Panadol and a rehydration ice block.
That was Thursday January 5 2017. Over the next six days his increasingly desperate parents returned to the hospital every day for the next five days, as Charlie’s condition deteriorated. But it wasn’t until Tuesday 10th January that he was finally admitted to hospital. By then, Charlie had a high fever, was wetting the bed and was so weak he had to be carried to the bathroom.
“I tried so hard to get my son the help that he needed. The hospital would not help him and there was nowhere else we could go,” his mother, Xernona PoiPoi, said in a statement.
Charlie was then flown to Cairns Hospital, where he was placed in an induced coma and flown to Brisbane. It was there that Charlie passed away on 14 January.
Astonishingly, Bamaga Hospital and the Torres Strait Cape Hospital and Health Service that governs it did not contact Charlie’s family to provide information about his death for 18 months.
His death was eventually subject to two internal reviews by the local health board, and a damning report from The Ombudsman in August 2020, which described “a substantial deficit” in Charlie’s care and found that although most people in the area identified as Aboriginal or Torres Strait Islander, the services at Bamaga Hospital were not culturally safe.
The Ombudsman’s report makes for heartbreaking reading, but George Newhouse, of the National Justice Project, who represents both the Gowa and Williams families, hopes that investigations into the two cases will signal change.
“Naomi William’s case was the first case where a judicial officer found that prejudice had contributed to the death of an Aboriginal or Torres Strait Islander person. Coroners in other states have been less willing to explore issues of systemic racism,” says Newhouse.
Naomi William’s case was the first case where a judicial officer found that prejudice had contributed to the death of an Aboriginal or Torres Strait Islander person
For Sharon Williams, the coronial process and findings were a vindication, and also presented a pathway forward to ensure “what happened to Naomi never happens to another family”.
Although the Williams family is working with NSW Health Minister and Murrumbidgee Health to ensure the coroner’s recommendations are implemented, she wants to see more accountability for those involved.
Prof Bond says that there needs to be accountability for the deaths of Aboriginal people within the health system, as well as an acknowledgement of the role of racism in their deaths.
“There’s a refusal to recognise that racism is real, or refusal to take responsibility for the violence of racism in the colony. They know it – the numbers speak to it in terms of 10 years less life expectancy, in the 20 times that a pregnant woman presents to hospital. Everyone is complicit in the silencing around conversations of race, and the silencing of blackfellas experiences of race.”
“We know racism. Our bodies feel it. And we know that feeling. But part of the psychological damage of racial violence is being told by everyone everywhere that we are just imagining it.”
For Sharon Williams, it is a violence that still enacts its own trauma on her and her family every day, with the absence of her daughter and her grandchild – who she should never have had to bury.
“She should still be here today. Our family will never be the same. And I haven’t got her here.”













1 Comment